PRP After Hair Transplant: What It Does, When to Get It, and How Many Sessions You Need
The question that comes up most often in post-op reviews is not about scabbing or sleeping positions. It is this: “Doctor, should I be getting PRP done?”
It usually surfaces around day 10, once the immediate anxiety of the procedure has passed and patients start reading everything they can find online. Some arrive convinced PRP is non-negotiable. Others have been told by a friend that it is just a money-making add-on.
Both positions are too simple. This article covers what PRP actually does to transplanted follicles, who genuinely benefits, when the sessions should happen, and how many you need — based on published clinical data and patterns observed in clinical practice.
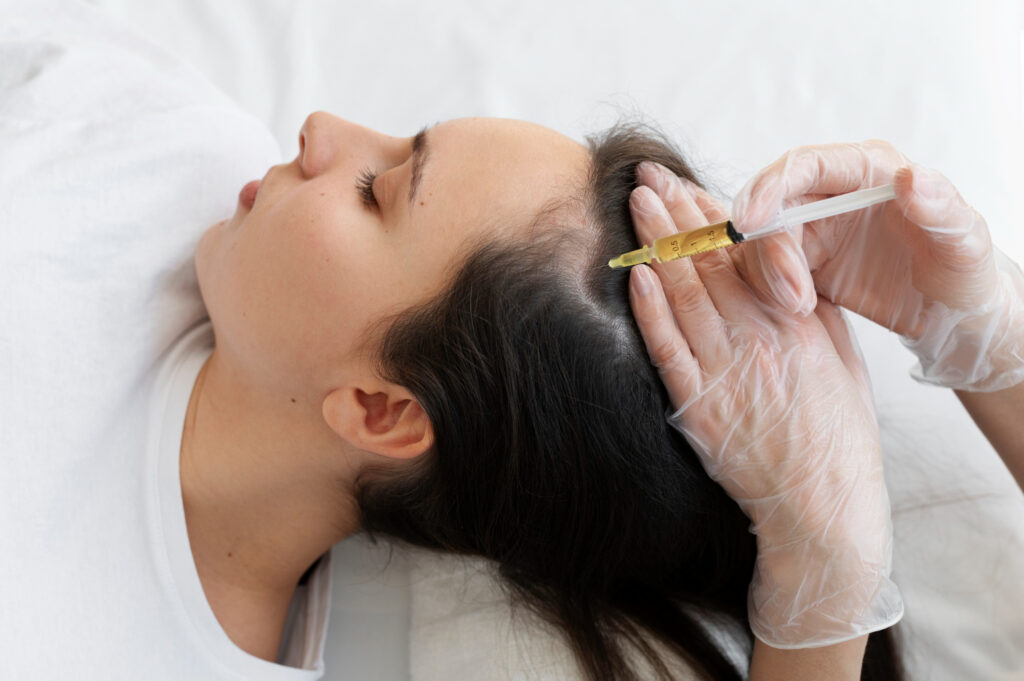
What Happens to Your Grafts in the First Few Weeks
Understanding why PRP matters or does not starts with understanding what transplanted follicles go through in the early weeks after surgery.
When follicles are extracted and reimplanted, they enter a period of roughly 72 to 96 hours where they have no blood supply. There are no capillaries connecting them to the scalp yet. They survive on diffusion — nutrients and oxygen moving slowly from the surrounding tissue. This is the graft survival window, and it is why how grafts are handled between extraction and implantation matters so much.
Once implanted and the surrounding tissue starts healing, the body’s normal wound response begins. Platelets aggregate at the wound site, growth factors are released, and new blood vessels start forming around the follicle roots. This process takes several weeks to complete.
Around weeks two to six, most patients notice that their transplanted hair starts shedding. This is called post-transplant shedding, or telogen effluvium, and it is completely normal. The hair shaft falls out, but the follicle itself remains in the scalp. It goes dormant — not dead. After a resting phase that typically lasts two to three months, the follicle re-enters the active growth phase (anagen) and new hair begins growing.
The issue is that in some patients, the shock of transplantation, combined with residual scalp inflammation, means some follicles do not recover as efficiently as they should. That is where PRP becomes relevant.
How PRP Works — The Biology, Not the Marketing
PRP stands for platelet-rich plasma. It is prepared from the patient’s own blood, no synthetic additives, no foreign substances.
The preparation process: 20 to 30 ml of blood is drawn, then placed in a centrifuge. The centrifuge spins the sample, separating it into three layers — red blood cells at the bottom, platelet-poor plasma at the top, and platelet-rich plasma in the middle. This middle layer is what is used. Platelet concentration in properly prepared PRP is typically three to five times higher than in whole blood.
Why does that matter for transplanted hair? Platelets contain granules packed with growth factors. Three are particularly relevant to follicle recovery:
PDGF (platelet-derived growth factor) — stimulates the dermal papilla cells, which sit at the base of each follicle and control the hair growth cycle. When dermal papilla cells are active, the follicle produces hair.
VEGF (vascular endothelial growth factor) — accelerates new blood vessel formation. For transplanted follicles sitting in tissue that is still re-establishing its blood supply, faster vascularization means better nourishment arriving sooner.
EGF (epidermal growth factor) — supports the regeneration of epithelial cells that form the outer root sheath of the follicle.
What PRP does, in short, is concentrate and deliver these signals directly to the area where the follicles are trying to establish themselves.
To be direct about the limits of the evidence: the data for PRP improving early graft survival conditions is solid. Claims about dramatically increasing long-term hair density from PRP alone — without accounting for graft count and surgical technique — are overstated.
Does PRP After a Hair Transplant Actually Make a Difference? What the Evidence Shows
There is real clinical data on this. Khatu et al. (2014), published in the Journal of Cutaneous and Aesthetic Surgery, showed statistically significant improvement in hair density scores in the PRP-treated group compared to controls. Gkini et al. (2014) reported a mean increase in hair density over a 12-month follow-up in patients receiving PRP.
More directly relevant to post-transplant use: several studies have examined PRP given intraoperatively — where grafts are soaked in PRP solution before implantation — and found improved graft survival rates, with some trials reporting a 10 to 15 percentage point improvement in the proportion of grafts that entered the growth phase by the six-month mark.
Clinical observation from practice indicates that patients who received PRP both during the procedure and in the three months following it consistently reached the early growth phase about four to six weeks sooner than those who did not. This is an observational pattern, not a controlled trial, and no causal conclusions are drawn from it. But it has been consistent enough that it warrants discussion during the post-op consultation for every patient who had more than 2,000 grafts placed.
Honest Limitations to Know About
PRP quality is not standardized across clinics. The platelet concentration you get depends on the centrifuge protocol, the tube type, and how carefully the plasma layer is separated. Poorly prepared PRP with low platelet concentration will not deliver meaningful growth factor concentrations regardless of the number of sessions. If the clinic preparing your PRP cannot tell you their average platelet count per session, that is worth asking about.
Results also vary by patient profile. Norwood Stage 5 or 6 patients with significant ongoing native hair loss show more variable outcomes from PRP on transplanted follicles alone. Younger patients with early-stage, stable hair loss may see the benefit largely attributable to good graft survival anyway.
When Should PRP Be Done — Before, During, or After?
There are three windows when PRP can be introduced, and they serve different purposes.
During the Transplant (Intraoperative PRP)
Extracted grafts are stored in a PRP solution rather than plain saline. This keeps follicles hydrated and exposes them to growth factors before they are even placed in the recipient zone. FUE procedures, where grafts can be out of the scalp for varying amounts of time, benefit from this more than FUT, where the strip is processed and implanted more quickly.
Post-Operative Sessions (One to Six Months)
The first month is when the scalp is most actively healing. The wound response is ongoing, new blood vessels are forming, and the follicles are either settling in or beginning to show stress. A PRP session at one month, once scabs have cleared and the scalp surface is intact, places concentrated growth factors directly into this active healing environment. The three-month session is timed around when many follicles are beginning to exit dormancy and re-enter anagen.
Addressing Native Hair Loss
Most patients who need a hair transplant have androgenetic alopecia that is still progressing. The non-transplanted hair in and around the recipient area is also miniaturizing. Post-operative PRP sessions can slow that miniaturization, which is why the treatment makes sense even when the transplant itself has gone well. The goal is not only to support new grafts but also to defend the existing hair around them.
How Many PRP Sessions Are Needed After a Hair Transplant?
The standard protocol, which is what the clinical literature generally supports, is three sessions in the first five to six months, spaced four to six weeks apart: first session at one month post-op, second at around three months, third at five to six months. After that initial course, one session every six months for the first two years works as maintenance for patients whose native hair loss is still progressing.
The timing is not arbitrary. The one-month session catches follicles during the transition from the wound-healing phase into early dormancy. The three-month session targets the period when many follicles begin re-entering anagen. The six-month session consolidates support as growth starts becoming visible.
If you miss the early sessions: The transplant will not fail. But the growth factor exposure that PRP provides during the healing window is time-sensitive. You cannot replicate a one-month session at month five and expect the same outcome.
Is more always better? Beyond four to five sessions in the first year, published data does not show compounding benefit. Three is the evidence-supported number for the initial course. Recommending six to eight sessions to every patient, regardless of their profile, is not a protocol that can be clinically justified.
Is PRP Necessary After a Hair Transplant Or Just Optional?
It is optional. A well-executed hair transplant, properly performed with appropriate graft handling, can produce good results without post-operative PRP. That is the honest answer, and patients should hear it.
That said, there are specific patient profiles where it is recommended clearly rather than left as a personal choice:
• Patients still actively losing native hair — Their miniaturized follicles respond to growth factor stimulation, and slowing native loss protects the visual density the transplant was meant to restore.
• Large graft sessions (3,000 grafts or more) — The vascularization demand on the scalp is higher, and PRP supports faster capillary formation across the larger recipient area.
• Fine or thin hair texture — Thinner follicles are more vulnerable to the shock loss phase. The growth factor support from PRP helps cushion that.
• Patients with impaired wound healing — This includes diabetic patients. The concentrated growth factors in PRP partially compensate for a slower native healing response.
Who may not need an extended course: Generally, a younger patient with stable, early-stage hair loss (Norwood 2–3), a small session under 1,500 grafts, and good scalp health going into the procedure is unlikely to gain much from a full three-session course.
What to Expect During a PRP Session
The session runs 45 to 60 minutes from blood draw to last injection.
After drawing 20 to 30 ml of blood, it goes into the centrifuge for a two-spin protocol — the first spin separates red cells, the second concentrates the platelet layer. While the sample is processing, a topical anesthetic is applied to the scalp and left on for 20 to 30 minutes. The prepared PRP is then drawn up and injected in a grid pattern across the recipient zone, and in the donor area if there is any post-operative concern there.
The injections cause brief, sharp stinging. Most patients find it manageable with the anesthetic in place. Some report mild scalp tenderness for the following 24 hours, which resolves on its own.
Post-session instructions: avoid washing the scalp for six hours, stay out of direct sunlight for 48 hours, hold off on vigorous exercise for 24 hours. No dietary restrictions, no extended recovery period.
PRP Compared to Other Post-Transplant Support Options
PRP is not the only tool available after a hair transplant, and knowing how it sits relative to the others helps patients make informed decisions.
PRP vs Minoxidil: Minoxidil works through vasodilation and potassium channel activity in the follicle, a completely different mechanism. It does not replace PRP. Most dermatologists introduce topical minoxidil at around the three-month mark, alongside PRP rather than instead of it.
PRP vs Finasteride: Finasteride addresses DHT-driven hair loss and is relevant for patients with progressive androgenetic alopecia. It does not directly affect graft survival or follicle recovery speed. Like minoxidil, it is complementary rather than interchangeable.
GFC (Growth Factor Concentrate): A newer variation some clinics now offer. The preparation is more standardized than conventional PRP, and the growth factor concentration is typically higher. Whether clinical outcomes are significantly better than well-prepared PRP is still being studied. If your dermatologist offers it, it is worth a specific conversation about their preparation protocol and what data they have for it.
Frequently Asked Questions
How soon after a hair transplant can I get PRP?
The first session is typically at one month post-op, once the scalp surface has healed, scabs have cleared, and there is no active inflammation or open skin.
How many PRP sessions are needed after a hair transplant?
The standard initial course is three sessions spaced four to six weeks apart, over the first five to six months. For patients with progressive hair loss, one maintenance session every six months for the first two years is generally recommended.
Is PRP painful after a hair transplant?
The injections cause brief stinging. With topical anesthetic applied beforehand, most patients find it tolerable. Mild scalp tenderness for 24 hours afterward is common and resolves on its own.
Can PRP make transplanted hair grow faster?
It can shorten the dormancy phase and bring follicles into the active growth phase earlier. Clinical observation suggests this is roughly four to six weeks earlier in patients who received both intraoperative and post-op PRP compared to those who did not. Individual results vary depending on follicle health, session size, and PRP preparation quality.
What is the cost of PRP after hair transplant in India?
Per-session costs typically range from ₹3,000 to ₹8,000 depending on the city and clinic. Package rates for the initial three-session course are commonly available.
Do I need PRP if I had an FUE hair transplant?
PRP is relevant for both FUE and FUT, the underlying follicle biology is the same. Whether a course is recommended depends on your session size, hair loss grade, and scalp condition, which is best assessed in a post-op review.
In Summary
PRP after a hair transplant is not a requirement for good results. It is a tool, one that works well in the right patient at the right time, with reasonable clinical evidence behind it, and one best recommended specifically rather than broadly.
If you have recently had a hair transplant and want to know whether a PRP course makes sense for your specific situation, the most useful step is a post-op review where scalp healing can be assessed, native hair loss activity checked, and a specific recommendation made.